Petechiae, purpura, and low platelets, when red dots on skin can signal urgency
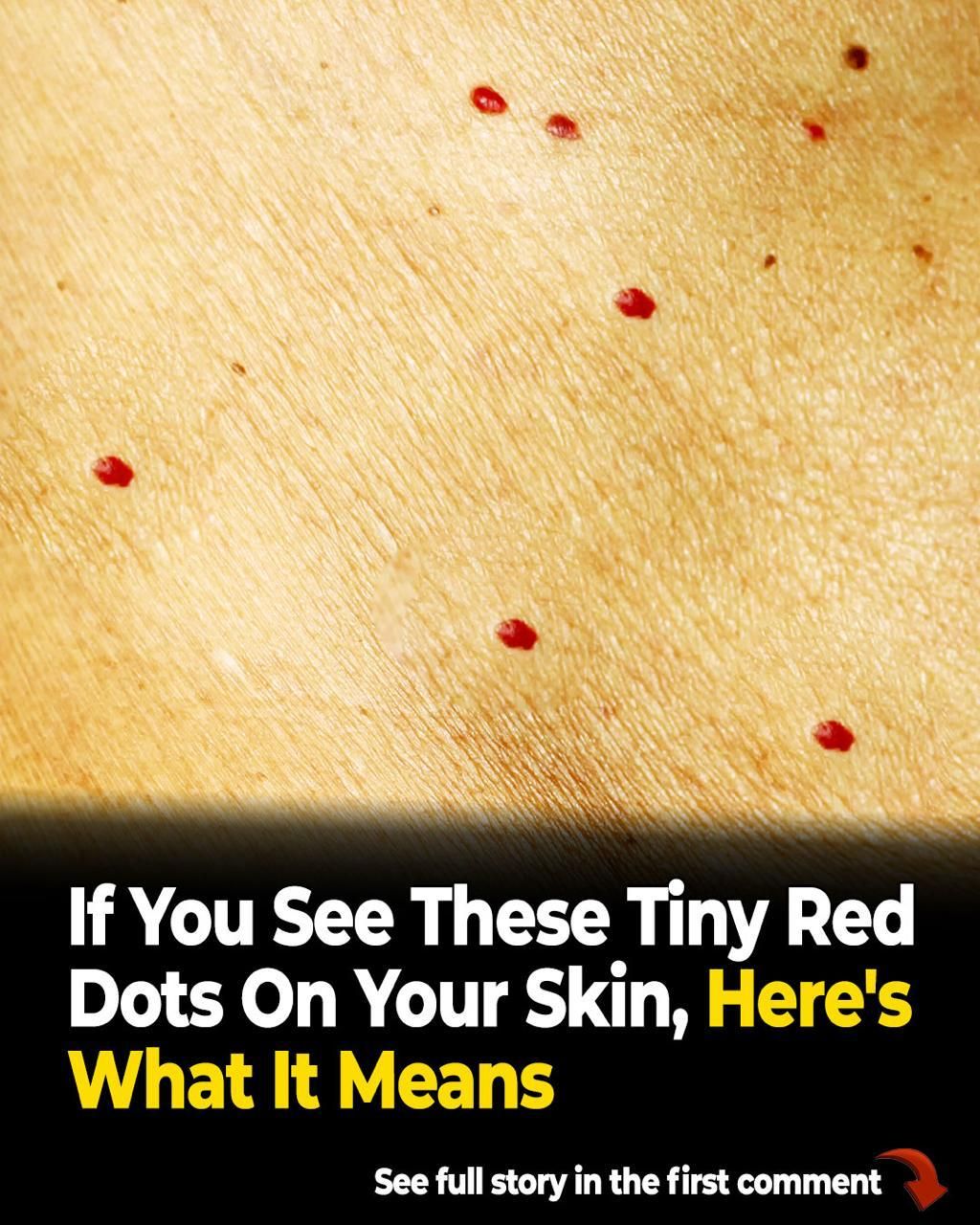
Petechiae look like tiny red or purple pinpoints that appear suddenly. They often cluster on the lower legs and ankles. Gravity increases pressure during standing and walking. Unlike a cherry angioma, petechiae do not rise above the skin surface. They also do not blanch with pressure because blood has leaked into the skin. states, “Areas of bleeding into the skin do not become paler (blanch) when you press on the area.” That clue helps. Timing and symptoms still matter. Clinicians use size terms that can help you describe what you see. StatPearls notes that petechiae measure less than 2 mm, while larger non-blanching spots are purpura. Petechiae can follow a clear trigger such as forceful coughing, vomiting, heavy lifting, or a long workout. In those cases, the dots often fade within days, and the person otherwise remains well.
Petechiae can also appear where clothing or straps create repeated pressure. A clinician still checks for bruises, gum bleeding, or heavy menstrual bleeding. Those signs can travel with low platelets. Petechiae can also reflect a platelet problem, and that possibility drives urgency. Platelets help blood clot, so a low platelet count can lead to pinpoint bleeding. NHLBI lists petechiae as a sign of immune thrombocytopenia. It defines them as “small, flat red spots under the skin caused by blood leaking from blood vessels.” Low platelets can follow illness or medicines. Immune disease can also play a role. They can also arise from bone marrow disease.
Clinicians avoid casual reassurance when the dots appear quickly, spread, or come with bruising that has no clear injury. Cleveland Clinic states: “If you have pinpoint-sized red dots under your skin that spread quickly, or petechiae plus other symptoms, seek medical attention.” Clinicians often order a complete blood count on the same day. They also review recent infections and medicines. Quick testing can show if the issue stays in the skin. It can also reveal a blood problem needing treatment. Even when tests are normal, the visit can rule out dangerous infections. It also gives a documented baseline for follow-up rash. If the dots appear on the whites of the eyes or inside the mouth, mention it immediately. Those sites can signal a wider bleeding tendency.
Clinicians also check for a rapidly spreading rash with fever, because some infections become dangerous fast. The CDC notes that meningococcal disease can include a petechial or purpuric rash, alongside sudden fever and other symptoms. If you cannot link the spots to a clear trigger, do not wait weeks to watch them. Mayo Clinic advises, “See a member of your health care team soon if you develop petechiae all over the body, or you can’t identify the cause of the petechiae.” Even when blood counts return to normal, the visit can still help. A clinician can confirm blanching, check vitals, and decide if you need follow-up testing. If you take blood thinners, ask whether dosing or interactions could contribute. If a child develops a non-blanching rash, treat it as a same-day assessment, unless a clear mechanical cause exists. Keep the photo timeline, because speed guides decisions.
Leave a Comment